Gaze Stabilization Exercises
Introduction
A key component of vestibular rehabilitation (VR) is gaze stabilization exercises. In order to improve the vestibular ocular reflex’s gain, enhance vision during head movement, and lessen vertigo and dizziness symptoms, they are often prescribed to patients with vestibular hypofunction.
This review will look at recent research that assessed the effectiveness of gaze stabilization exercises on oscillatory vision, dynamic visual acuity, and VOR gain. Additionally, newer types of gaze stabilization exercises and recent experimental studies using digital technologies will be reviewed. There will be a discussion of the implications for VR research and future clinical practice.
What is Gaze Stabilization?
- Through gaze stabilization, affected people can concentrate on a single object at a time without experiencing vertigo or nausea. Patients who suffer from vertigo, dizziness, or other vestibular problems can benefit from this physical therapy technique. It can be challenging for someone’s eyes to stay focused while their head or body moves when their balance system is malfunctioning.
- Gaze stabilization improves the ability to focus on stationary or moving objects without feeling lightheaded or unsteady by retraining the brain and eyes to work together. Whether a person is recovering from a particular vestibular disorder or managing a chronic condition, this technique is essential in helping them regain control over their balance.
What Do Gaze Stabilization Exercises Do?
- By learning how the brain and eyes cooperate, gaze stabilization exercises help people regain their balance and reduce feelings of vertigo. These exercises usually require moving the head in various directions while maintaining focus on a stationary object. They enable you to stabilize your vision while moving by gradually assisting your brain in adjusting to the input from your eyes and inner ear.
- As patients develop, the exercises are made more difficult by adding quicker motions, focusing on objects at varying distances, or switching up the background to assess visual focus in various scenarios. In the end, gaze stabilization exercises enhance your capacity to keep your eyes steady even in challenging situations.
To stabilize gaze in relation to space, the Vestibulo-ocular reflex (VOR) produces compensatory eye movements of equal and opposite magnitude to head rotation. Due to impaired VOR function, patients with compromised vestibular systems are more likely to fall, have poor balance and postural control, and have blurry vision.
Previous randomized and controlled studies have shown moderate to strong evidence of these exercises’ effectiveness. Gaze stability exercises have recently been validated for patients with multiple sclerosis, motion sickness, and fear of falling. The exercises did not specifically call for fixation on stationary or moving targets during head rotations; this is an improved version of those exercises.
Each kind provides a chance to investigate the weaknesses brought on by vestibular loss and the compensatory mechanisms that patients use to keep their gaze stable while moving their heads. n fact, no previous research has measured the dynamic patterning of head movements during gaze-stabilization exercises or evaluated whether vestibular loss affects this patterning.
Therefore, we examined whether subjects’ head movement patterns during gaze-stabilization exercises are affected by unilateral vestibular loss. In order to do this, we first looked at how people incorporate vestibular feedback in real time to modify their future movements. Next, we evaluated the temporal regularity of head motion using sample variability.
We discovered that, in contrast to controls, vestibular-loss patients make less flexible and more stereotyped head movements. Our findings offer the first experimental proof that head movement patterning is a useful indicator for identifying people with vestibular impairment, providing fresh information that may help guide patient rehabilitation.
Vestibular disorders
The “vestibular” system refers to the inner ear system with its fluid-filled canals that facilitate balance and spatial orientation. Vestibular neuritis and nerve compression are a few common vestibular disorders. Vestibular dysfunction can be bilateral, affecting both sides of the body, or unilateral, affecting just one.
Benign Paroxysmal Positional Vertigo (BPPV) is the most well-known vestibular condition. A brief dizzy feeling accompanied by blurred vision in relation to specific head positions is the hallmark of Benign Paroxysmal Positional Vertigo. Anterior, posterior, or horizontal vestibular canals may be impacted by Benign Paroxysmal Positional Vertigo .
According to published research, 80% of patients with Benign Paroxysmal Positional Vertigo have the posterior canal, which is the most frequently affected canal. Which canal is impacted by Benign Paroxysmal Positional Vertigo may be determined by several positional tests, including the Dix-Hallpike, supine roll, and head-shaking nystagmus tests.
The symptoms of vestibular damage are often chronic and irreversible. Vestibular rehabilitation enhances the compensatory process to reduce both primary and secondary symptoms, even though the body naturally compensates for vestibular dysfunction (as it does for the dysfunction or deficiency of any sense).
Vestibular suppressants prevent the nervous system from compensating in cases of chronic vestibular dysfunction. Therefore, people with chronic vestibular dysfunction cannot benefit from long-term medication. For long-term vestibular dysfunction, vestibular rehabilitation therapy is therefore a better choice. However, some drugs, like benzodiazepines, anticholinergics, and antihistamines, can help reduce nausea and other secondary symptoms in acute cases (less than five days).
Rotational chair testing
This test measures the degree to which the central nervous system (CNS) responds to bilateral vestibular hypofunction. The relationship between head velocity and eye movement is caused by endolymph, a fluid that moves inside the inner ear.
A patient is placed in a rotating chair, the chair is rotated to a specified speed, and eye movement is monitored. The velocity of eye movement should be equal to and opposite that of head movement in people with normal vestibular function. The degree of CNS compensation is evaluated using lower rotational velocities.
Visual perception testing
With a limited level of specificity, visual perception tests can evaluate a patient’s capacity to identify objects that are oriented both vertically and horizontally. A person with normal vestibular function can align a bar within 2.5 degrees of either horizontal or vertical when asked to do so. Vestibular dysfunction is indicated by an inability to do so. Sometimes the dysfunction is on the same side as the direction of tilt away from the intended orientation, and other times the opposite is true.
Diagnostic tests
Each patient must be thoroughly assessed in order to diagnose vestibular dysfunction and select the appropriate exercises for treatment because vestibular rehabilitation therapy approaches vary depending on the type of vestibular dysfunction, ability level, and history of symptoms.
In order to treat inner ear dysfunctions and retrain the brain for improved functionality, vestibular physiotherapy uses precise movements and sports with the goal of improving stability and reducing vertigo. Benign paroxysmal positional vertigo (BPPV), a common vestibular condition, can be effectively treated with these repositioning techniques.
Vestibular rehabilitation might not be the best course of action in certain situations. A person’s ability to maintain posture, balance, and head position is one of the many assessments that can be used to diagnose vestibular disorders. Certain diagnostic tests are easier to administer in a clinical setting than others, but they provide the tester with less exact information, and vice versa.
The symptoms’ nature, frequency, and circumstances—including whether they are triggered or spontaneous—should all be included in a thorough history of symptoms. Vestibular rehabilitation therapy can also be used to treat multiple sclerosis patients’ vertigo and concussion symptoms. Regardless of whether vestibular rehabilitation is a viable treatment option, magnetic resonance imaging techniques can be utilised as diagnostic tools to identify any problems.
Caloric reflex test
The caloric reflex test was created to assess vestibular system function and identify the root cause of vestibular symptoms. Pouring water into the patient’s external auditory canal and watching for nystagmus, or involuntary eye movement, is the reflex test. The direction of eye movement is influenced by the water’s temperature when vestibular function is normal. This condition is not present in people with peripheral unilateral vestibular hypofunction.
Different patterns of posturography can be identified by using a variety of technologies to evaluate an individual’s capacity to maintain balance and posture. The modalities and inputs that the individual uses to keep their balance can be established once a pattern has been identified. It is possible to identify various areas of dysfunction and preference by identifying the systems and structures that shape an individual’s position.
Non-vestibular dizziness
Vestibular symptoms, particularly balance problems and potentially dangerous falls, can occur in patients whose vestibular test results are normal. Concussions, Parkinson’s disease, cerebellar ataxia, normal-pressure hydrocephalus, leukoaraiosis, progressive supranuclear palsy, and large-fibre peripheral neuropathy are a few conditions that can cause non-vestibular dizziness. Additionally, several conditions are referred to as chronic situation-related dizziness disorders.
As an example, phobic postural vertigo (PPV) happens when a person with obsessive-compulsive traits feels unbalanced even when there are no balance problems. Similar symptoms include persistent vertigo, hypersensitivity to motion stimuli, and trouble with precise visual tasks in chronic subjective dizziness (CSD). Vestibular rehabilitation therapy or other therapeutic approaches like cognitive behavioural therapy may be used to treat both phobic postural vertigo and persistent subjective dizziness.
Gaze stabilisation exercises
Tips
- While the head is moving, the target must appear stationary, stay in focus, and not become blurry.
- Exercise by moving your head 45 degrees to either side of your midline.
- As long as the target is still in focus, the head motion should be accelerated.
- Wear your glasses if you wear them when working out.
- Reduce your head movement a little if you feel too lightheaded. Take a break in between each workout. Exercises require focus; stay away from distractions.
- Standing exercises must be done next to someone or near a counter for safety.
- Improvement in vision and the capacity to concentrate on a stationary object while the head is moving are the goals of gaze stabilisation exercises.
- The exercises that are appropriate for you should be determined by your therapist.
- Look directly ahead and concentrate on a letter that is held at eye level in front of you, such as an “E.”
- Keep your eyes on the target letter as you move your head towards it. Increase the speed at which your head moves. Maintaining the letter’s focus is essential. Slow down if you feel too feeling dizzy.
- Start performing the exercise for as long as it causes mild to moderate symptoms (you could use the number rating scale).
Start performing the exercise for as long as it causes mild to moderate symptoms (you could use the number rating scale). This could last for just ten seconds. You can gradually increase the duration to one minute (the brain requires this time to adjust). Gradually increase the frequency to three to five times per day.
This exercise can also be performed with an up-and-down (nodding) motion.
Putting the target letter on a busy background is one way to advance this exercise. The exercise should begin while you are seated and progress to standing.
1. In bed or sitting
A. Eye movements
- Both up and down
- From side to side
- concentrating on the finger’s movement from three feet to one foot away from the face
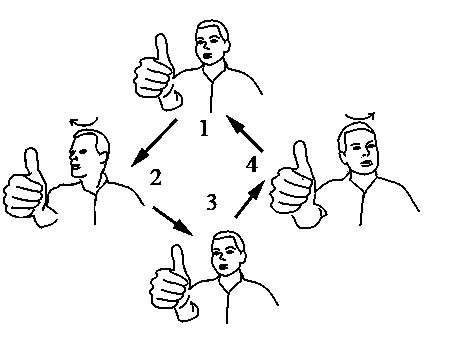
B. Head motions
- Bending both forward and backward
- Shifting back and forth
2. Sitting

- A. Head and eye movements
- B. Circle your shoulders and shrug.
- C. Reach forward and retrieve items from the floor.
- D. Lift items off the ground by bending side to side.
3. Standing

- A. Motions of the head, shoulders, and eyes
- B. Move from a sitting to a standing position while keeping your eyes open, then close them (please be aware that this is not recommended for older people with postural hypertension).
- C. Throw a ball above eye level from hand to hand.
- D. Under the knee, toss a ball from hand to hand.
- E. Turn around as you move from a seated to a standing position.
4. Moving about

- A. Climb and walk down a hill
- B. Climb and descend stairs
- C. Launch and retrieve a ball
- D. Any game (like bowling) that requires bending, stretching, and aiming
What Conditions Can Gaze Stabilization Exercises Treat?
A variety of vestibular disorders that affect balance, coordination, and spatial orientation can be effectively treated with gaze stabilization exercises. Problems with the inner ear or the brain’s processing of balance signals are frequently the cause of these disorders. Gaze stabilization is beneficial for several conditions, including:
Vestibular neuritis
This condition is brought on by inflammation of the vestibular nerve, which results in quick and acute vertigo. Vestibular neuritis causes imbalance, spinning sensations, and difficulty focusing. Gaze stabilization enables patients to regain stable vision as they heal by instructing the brain and eyes to cooperate.
Central vestibular disorders
The central nervous system’s capacity to process balance information is impacted by these neurological disorders. Dizziness and unsteady vision can result from disorders like multiple sclerosis, brain injuries, or stroke that interfere with the brain’s coordination with the eyes. In order to help patients regain control over their visual focus while adjusting to these disruptions, gaze stabilization exercises are essential.
Acoustic neuroma
The vestibulocochlear nerve (cranial nerve VIII), which is in charge of hearing and balance, is where this benign tumor grows. Dizziness, hearing loss, and trouble focusing can result from the tumor’s growth interfering with balance signals. By assisting patients in regaining control over their vision, gaze stabilization enhances their capacity to stay balanced while moving.
These are only a handful of the numerous circumstances where gaze stabilization is advantageous. By retraining your brain to rely on visual inputs for balance and spatial awareness, the exercises will eventually help you feel less lightheaded and have better coordination. Gaze stabilization exercises are a tried-and-true way to restore functional vision and balance, regardless of whether the condition is caused by a problem with the central nervous system or inner ear.
What Conditions Aren’t Helped by Gaze Stabilization?
Although gaze stabilization works well for many vestibular disorders, there are some situations in which it isn’t as beneficial. Benign Paroxysmal Positional Vertigo (BPPV), the most prevalent kind of vertigo, is a common condition.
When microscopic calcium particles in the inner ear come loose and interfere with the balance signals that are transmitted to the brain, BPPV happens. Since BPPV is frequently treated with repositioning maneuvers to move the particles back into place, gaze stabilization isn’t usually the best way to address this problem.
Gaze stabilization exercises may not be necessary for other sudden causes of vertigo, such as migraines or anxiety-induced dizziness. In these situations, the feeling of dizziness usually goes away on its own or with other particular treatments.
Physical therapists may still recommend gaze stabilization to help patients practice focusing and lessen symptoms of dizziness, even in situations where it isn’t the main course of treatment. This can help patients regain stability in their everyday activities and enhance their general balance.
FAQs
Do gaze stabilization exercises work?
A variety of vestibular disorders that affect balance, coordination, and spatial orientation can be effectively treated with gaze stabilisation exercises. Problems with the inner ear or the brain’s processing of balance signals are frequently the cause of these disorders.
How to do gaze stabilization exercises?
Focus on a letter (like an ‘E’) that is held at eye level in front of you while looking straight ahead. Keep your eyes on the target letter as you move your head back and forth. Increase the speed at which your head moves. Maintaining the letter’s focus is essential.
What is gaze stability?
The ability to keep looking while moving the head is referred to as gaze stability. The patient is seated to begin the evaluation. As the patient actively rotates his head to the right, then to the left, the therapist gives him instructions to keep his eyes on a fixed target.
How to reset your brain after vertigo?
Bend your head to look at the floor while seated, then raise it to look at the ceiling.
Lead your head while keeping your eyes fixed on the ceiling and the floor.
Do this ten times. Stop and give the symptoms 30 seconds or so to go away.
Repeat the entire procedure twice more.
What is the most effective exercise for vertigo?
Exercises by Brandt-Daroff (for BPPV)
Start by sitting down.
Lie down quickly on one side and turn your head to face the ceiling at a 45-degree angle.
Hold until the vertigo goes away, about 30 seconds.
Spend 30 seconds sitting down again.
On the opposite side, repeat the procedure.
Even after symptoms subside, continue to perform twice a day, five times on each side.
Exercises for gaze stabilisation
Focus on a point in front of you while sitting or standing, then quickly move your eyes to a nearby object.
Head turns: Move your head back and forth while maintaining eye contact with a single, still object.
Walking with head turns: Look in the direction of your step as you walk. Look right, for instance, when you step with your right foot.
Do eye exercises actually work?
What eye exercises can and cannot do
They might reduce eye fatigue and strain.
Boost focus, eye-hand coordination, and eye-muscle coordination.
Encourage blinking to help with dryness caused by screen time.
Tone and strengthen your eye muscles.
It is useful as a component of vision therapy for disorders that can impair reading, such as convergence insufficiency.
Since nearsightedness, farsightedness, and astigmatism are caused by the shape of the eye rather than weak muscles, they are unable to correct these refractive errors.
Get eliminated of the need for contact lenses or glasses.
Treat severe eye conditions like macular degeneration and glaucoma.
What is the 30 second eye exercise?
Palming: A 30-Second Eye Relaxation Retreat
To begin, warm your palms by rubbing them together. With your fingers pointing upward toward your forehead, gently place the palms of your hands over your eyes. Cover your eyes and unwind. You are free to go longer, but we prefer to count to thirty.
Which exercise is best for eyesight?
Reduction of tension and relaxation
Palming: Gently cover your closed eyes with your palms without applying pressure after rubbing your hands together to create warmth. To lessen eye strain, relax by taking deep breaths for 30 to several minutes.
Blinking: To keep your eyes hydrated and less dry, especially when staring at a screen, blink ten times per minute.
The 20-20-20 rule: To avoid digital eye strain, look at something 20 feet away for 20 seconds every 20 minutes.
Increasing flexibility and strengthening eye muscles
Roll your eyes slowly in a full circle, first clockwise and then counterclockwise, while sitting upright. In each direction, repeat five to ten times.
Focus both close and far away: Keep your finger a few inches away from your face and concentrate on it. Next, turn your attention to something on the other side of the room. Do this back and forth multiple times.
Figure 8: Imagine a big figure eight ten feet away on the wall. To enhance your coordination, trace the shape with your eyes for approximately thirty seconds while moving in both directions.
References
Eye exercises. (n.d.). DHMC and Clinics. https://www.dartmouth-hitchcock.org/otolaryngology/eye-exercises
Meldrum, D., & Jahn, K. (2019). Gaze stabilisation exercises in vestibular rehabilitation: review of the evidence and recent clinical advances. Journal of Neurology, 266(S1), 11–18. https://doi.org/10.1007/s00415-019-09459-x
RKadmin. (2025, March 7). What is Gaze Stabilization, and How do Physical Therapists Use This Technique? Core 3 Physical Therapy. https://core3pt.com/what-is-gaze-stabilization/
Vestibular (Balance) Exercises – University of Mississippi Medical Center. (n.d.). https://umc.edu/Healthcare/ENT/Patient-Handouts/Adult/Otology/Vestibular_Exercises.html
VOR exercise / Gaze stabilisation exercises – ear, balance and eustachian tube. (n.d.). https://earandbalance.co.uk/vor-exercise-gaze-stabilisation-exercises/